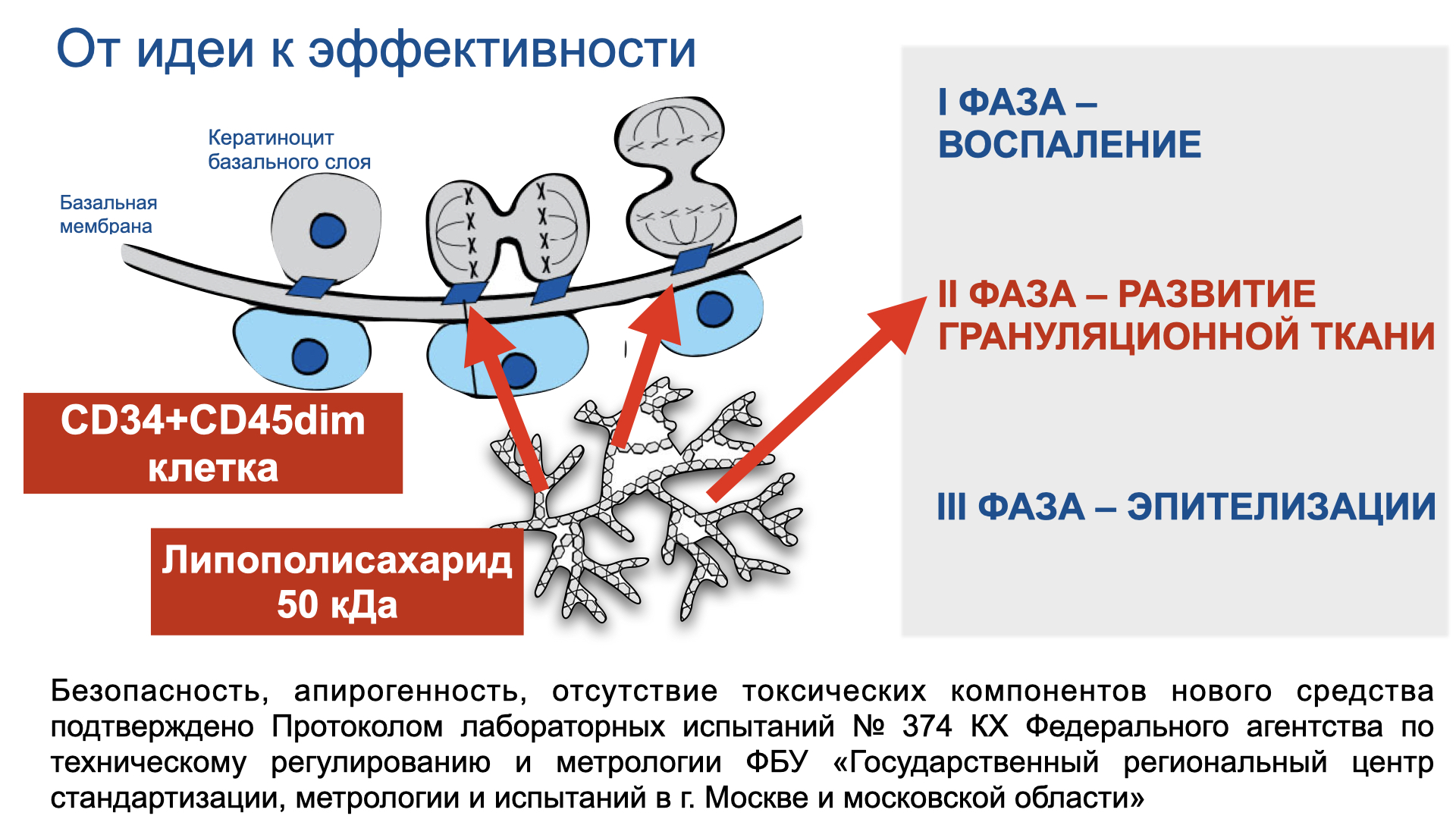
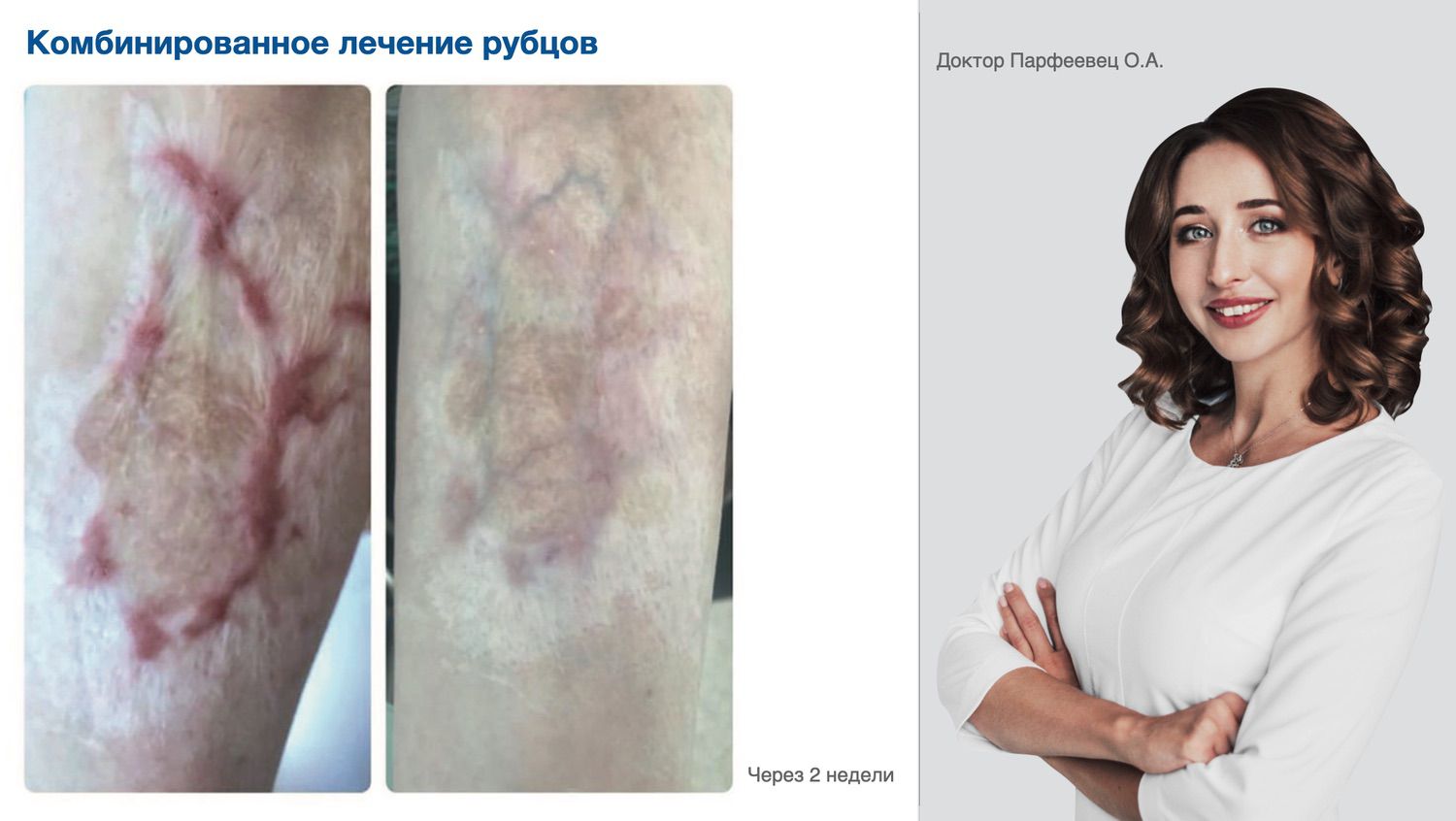
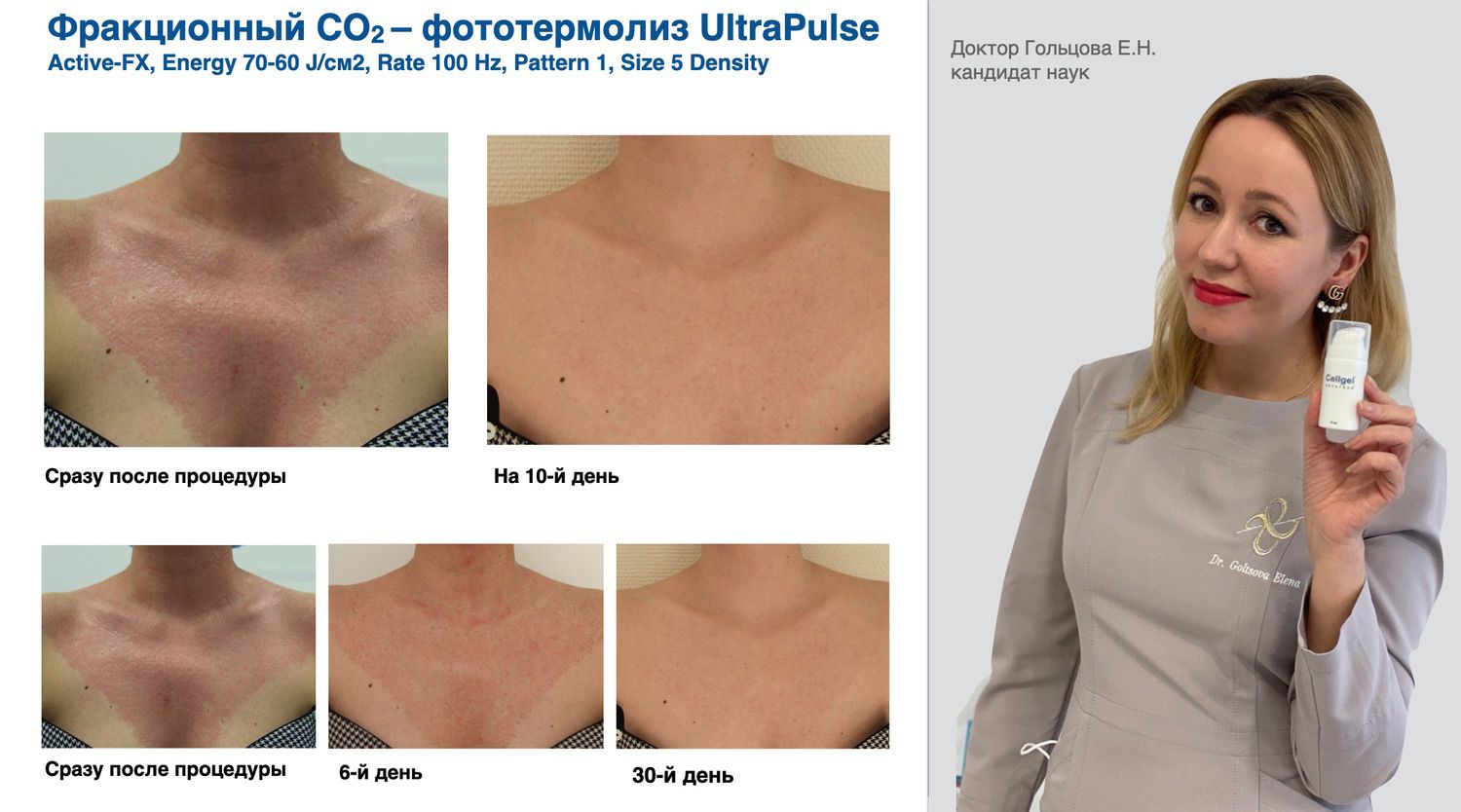
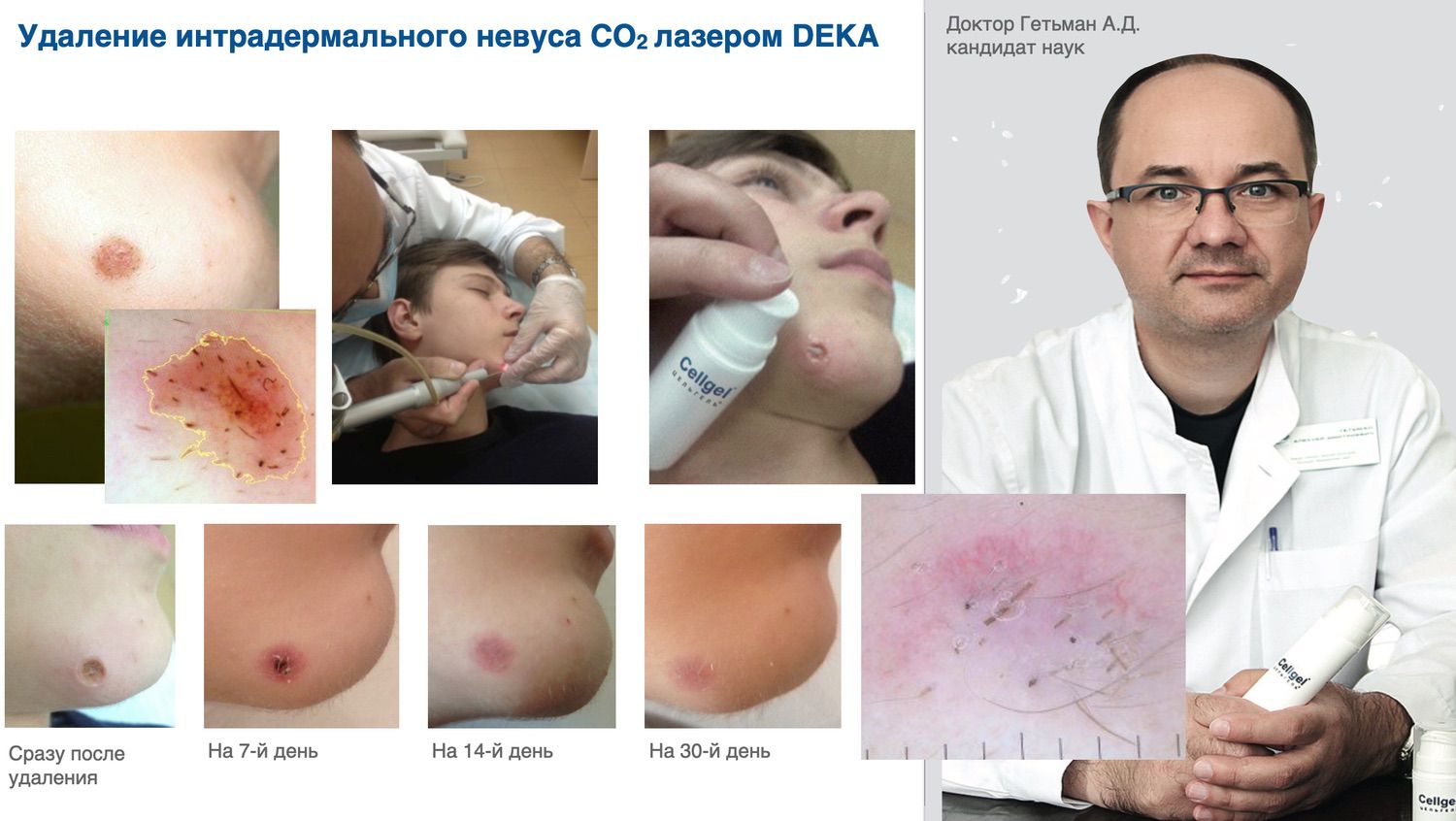
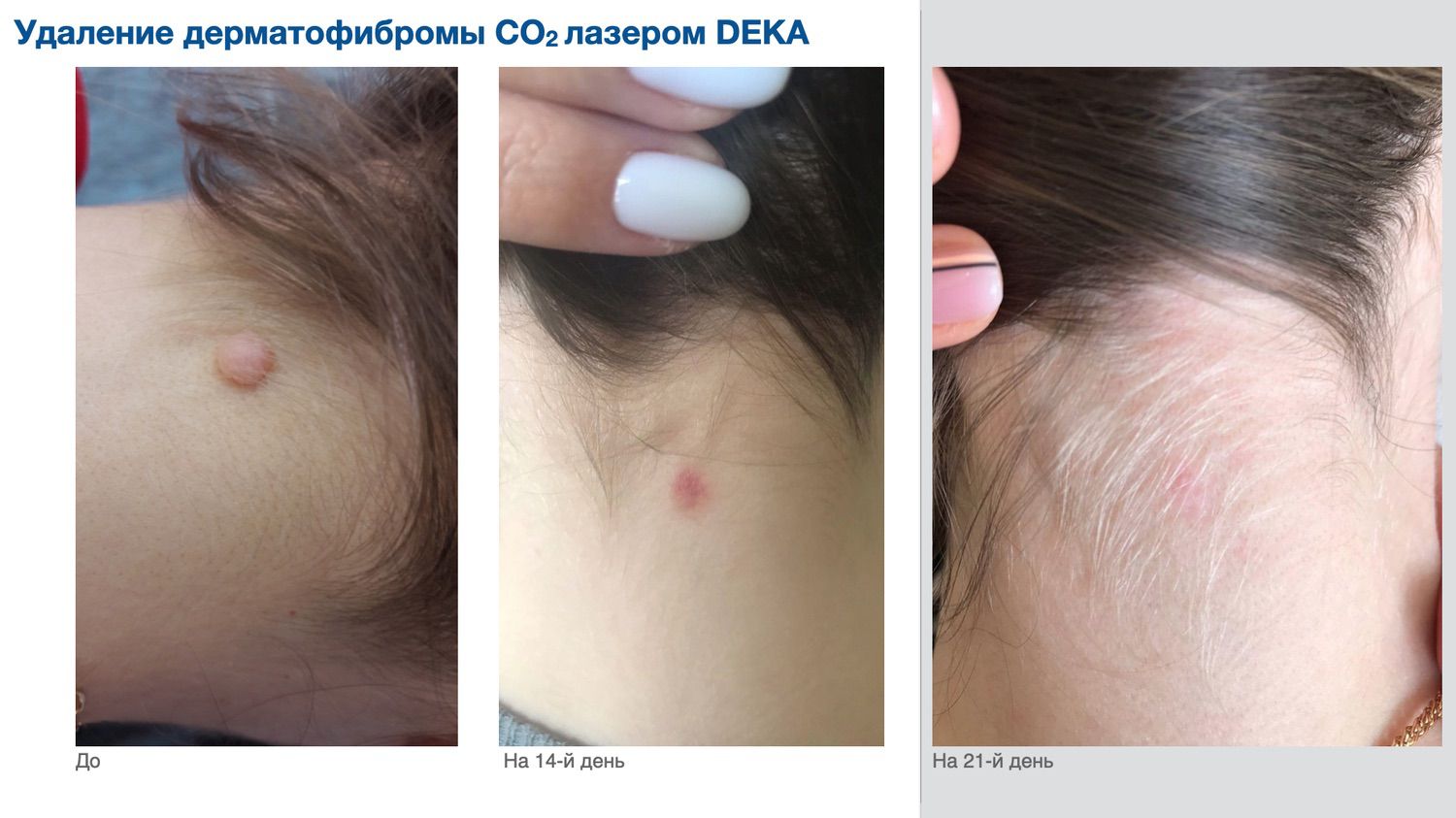
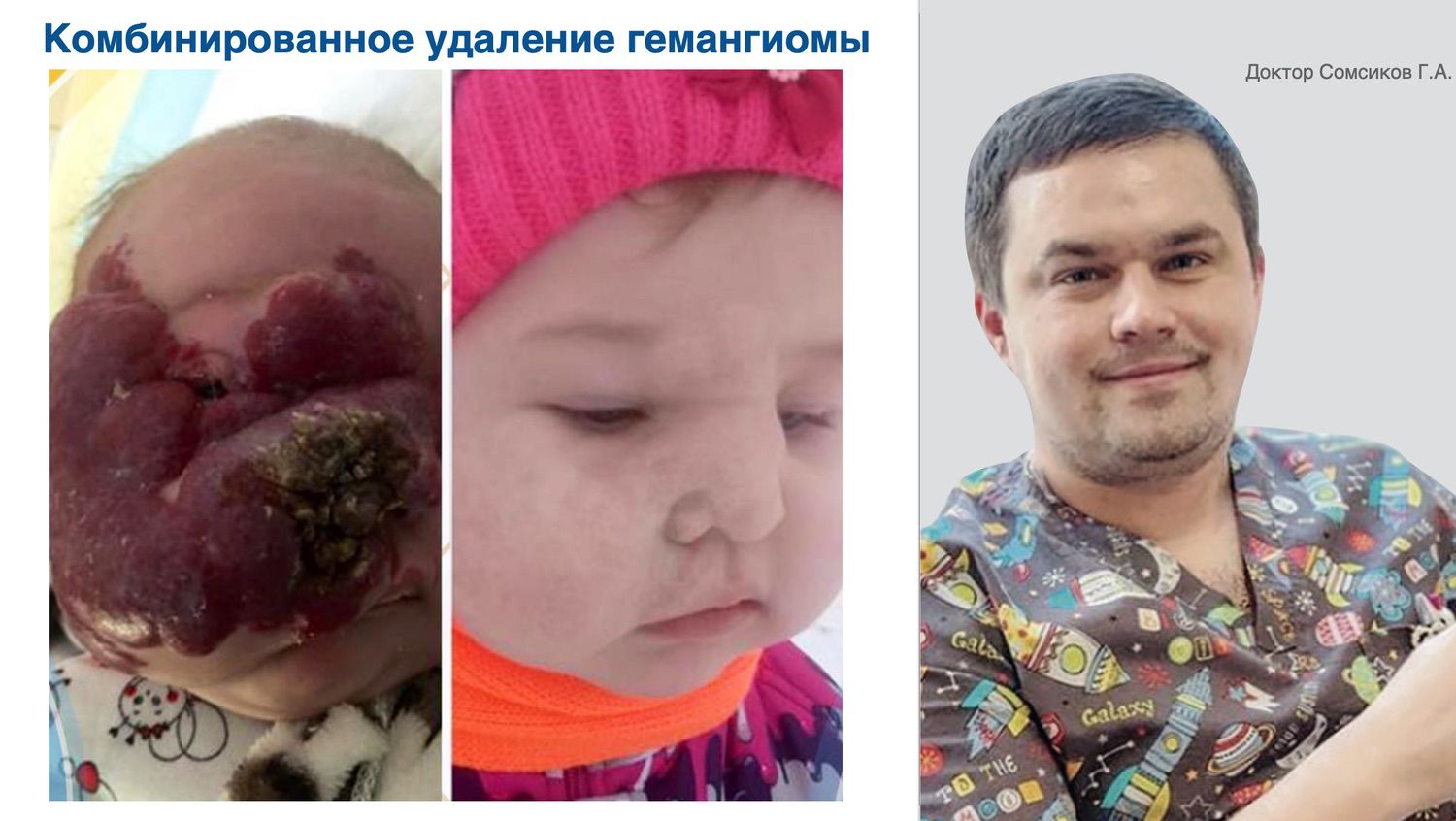
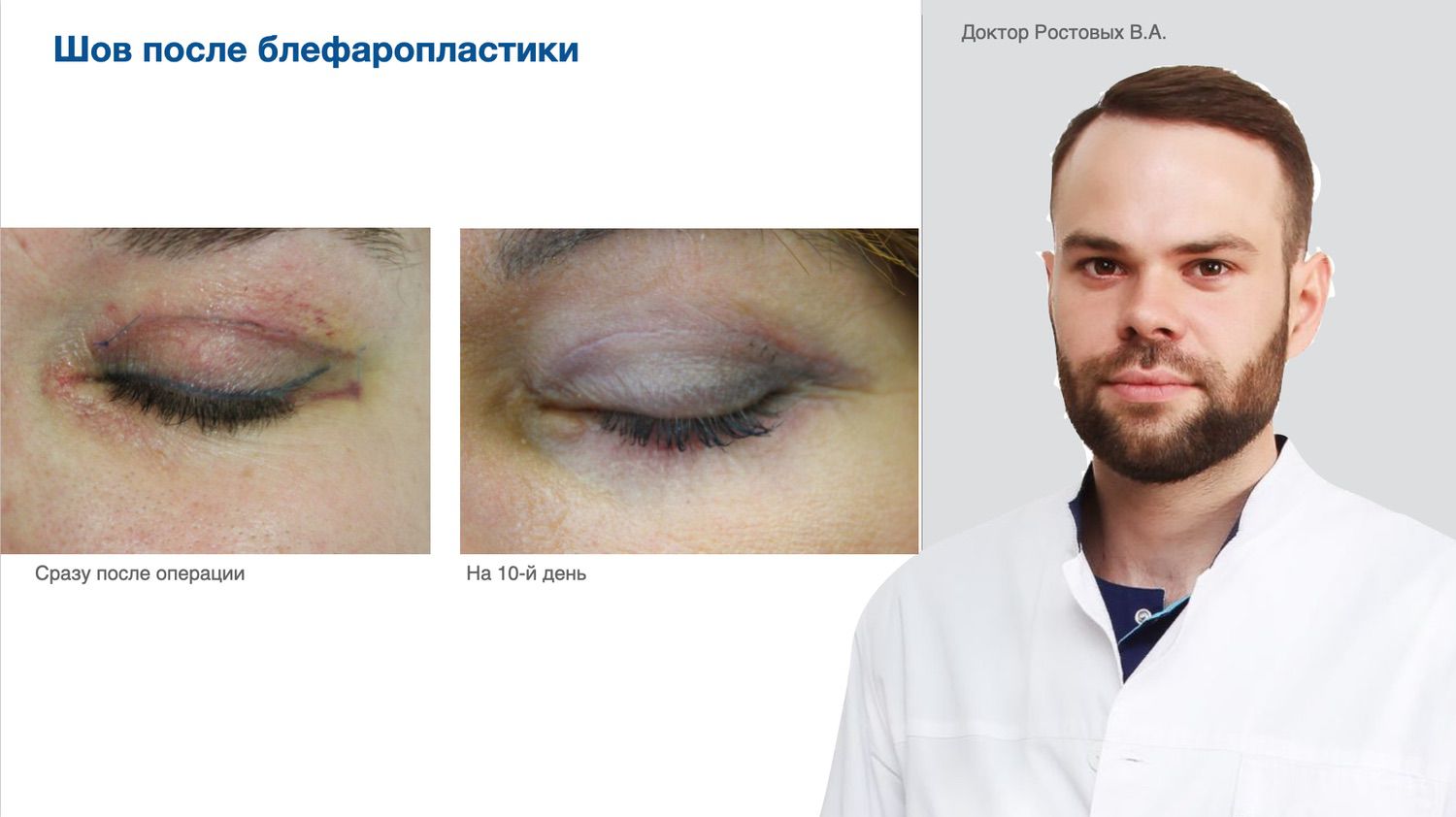
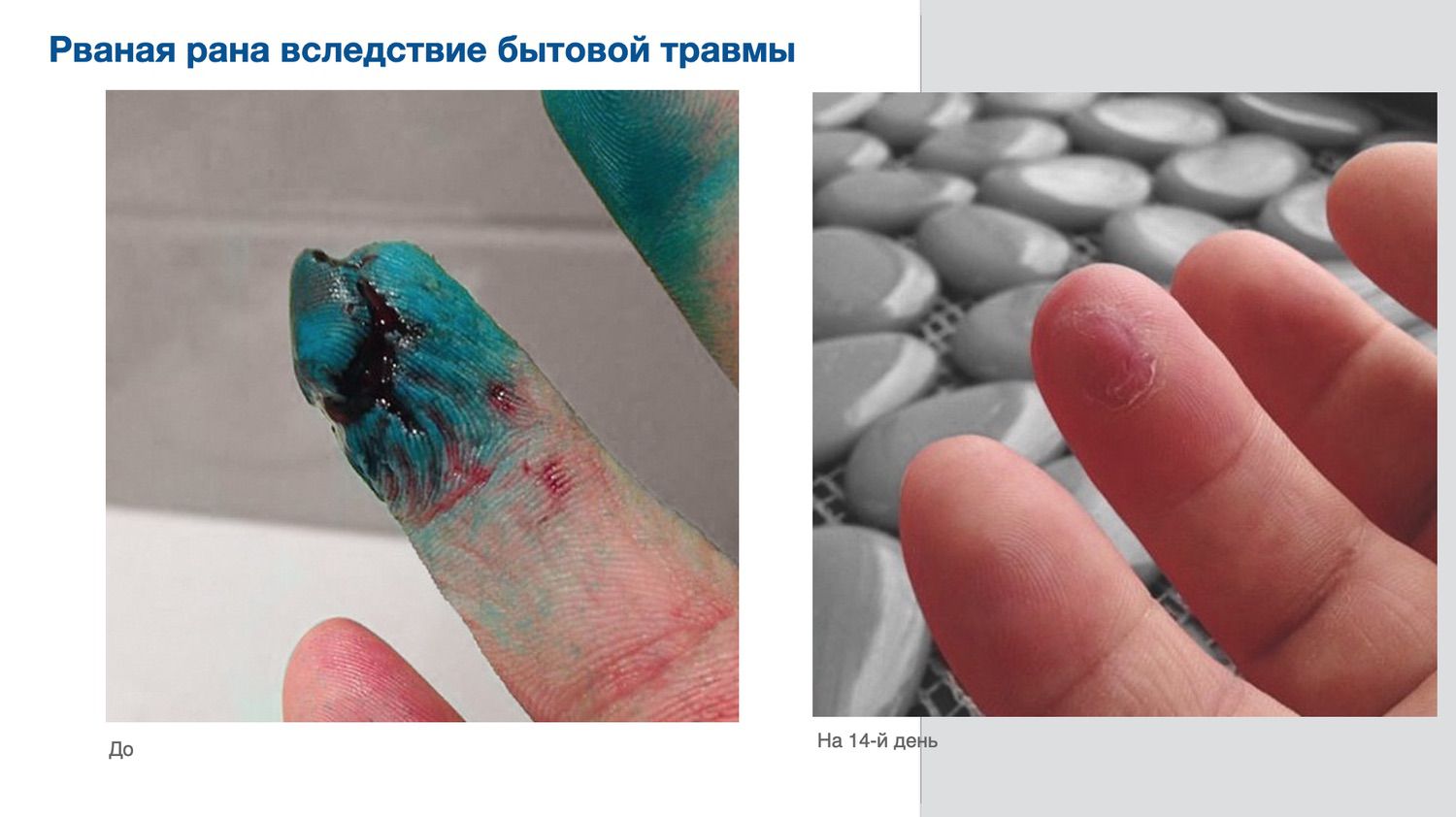
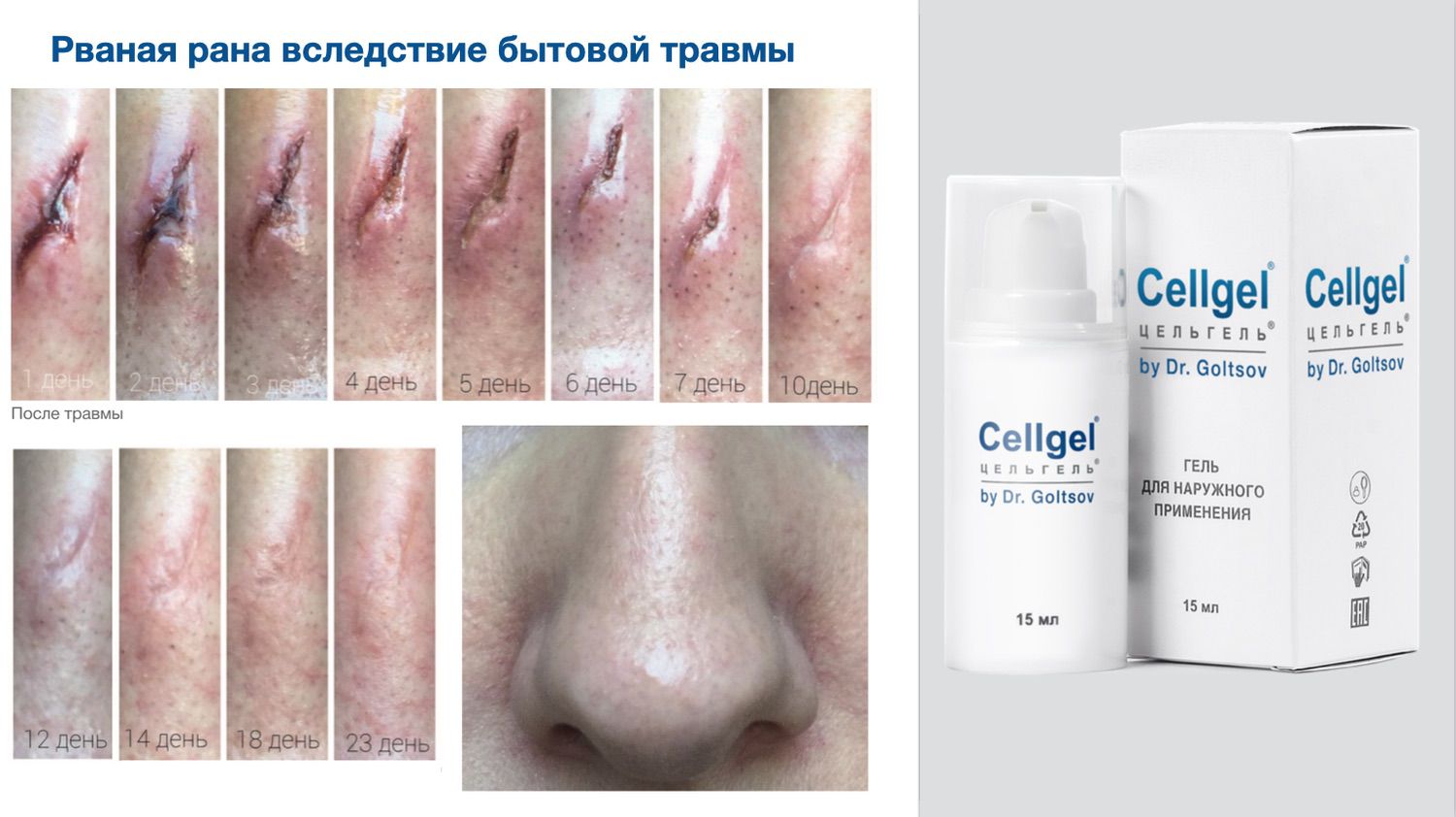
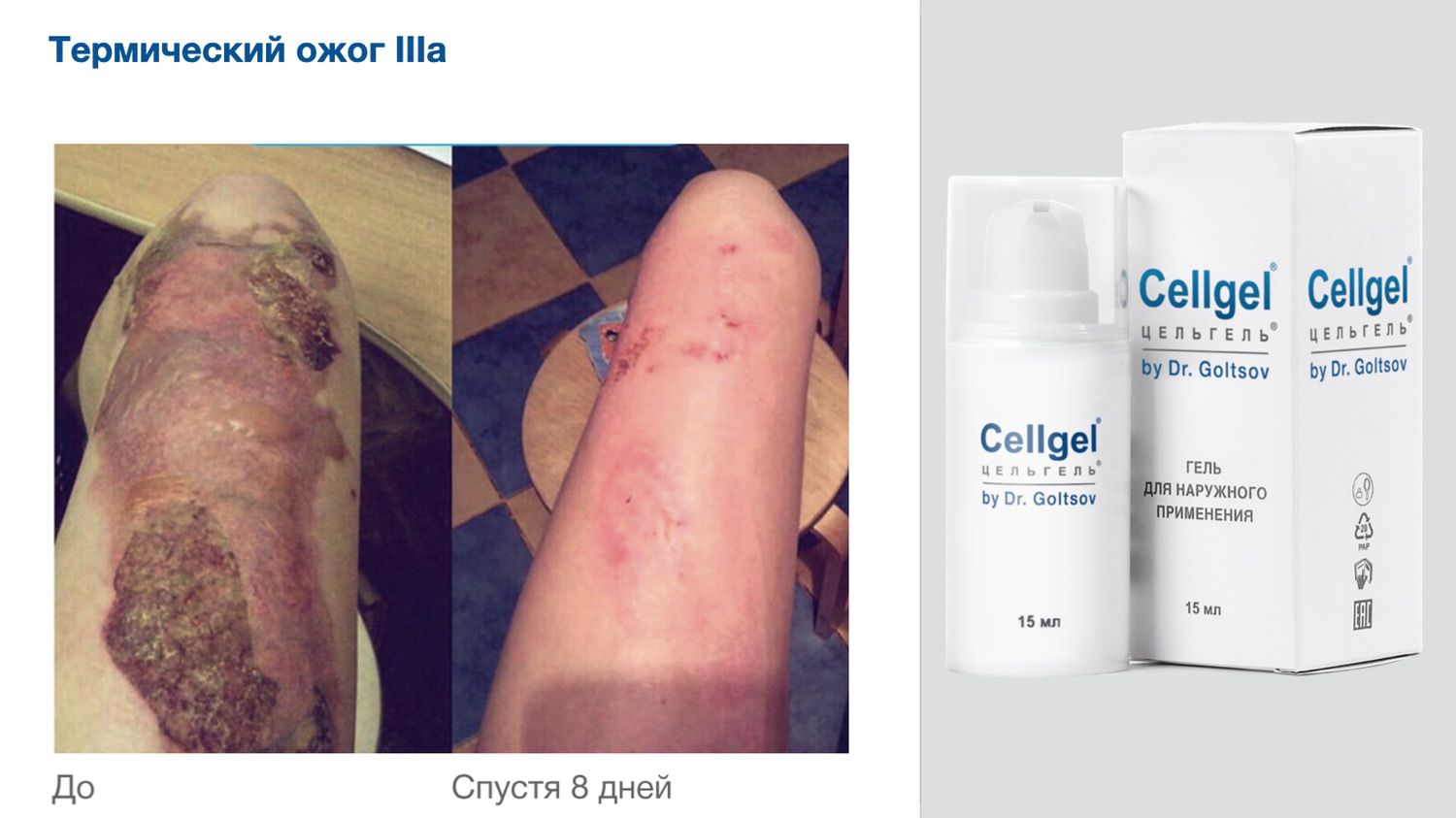
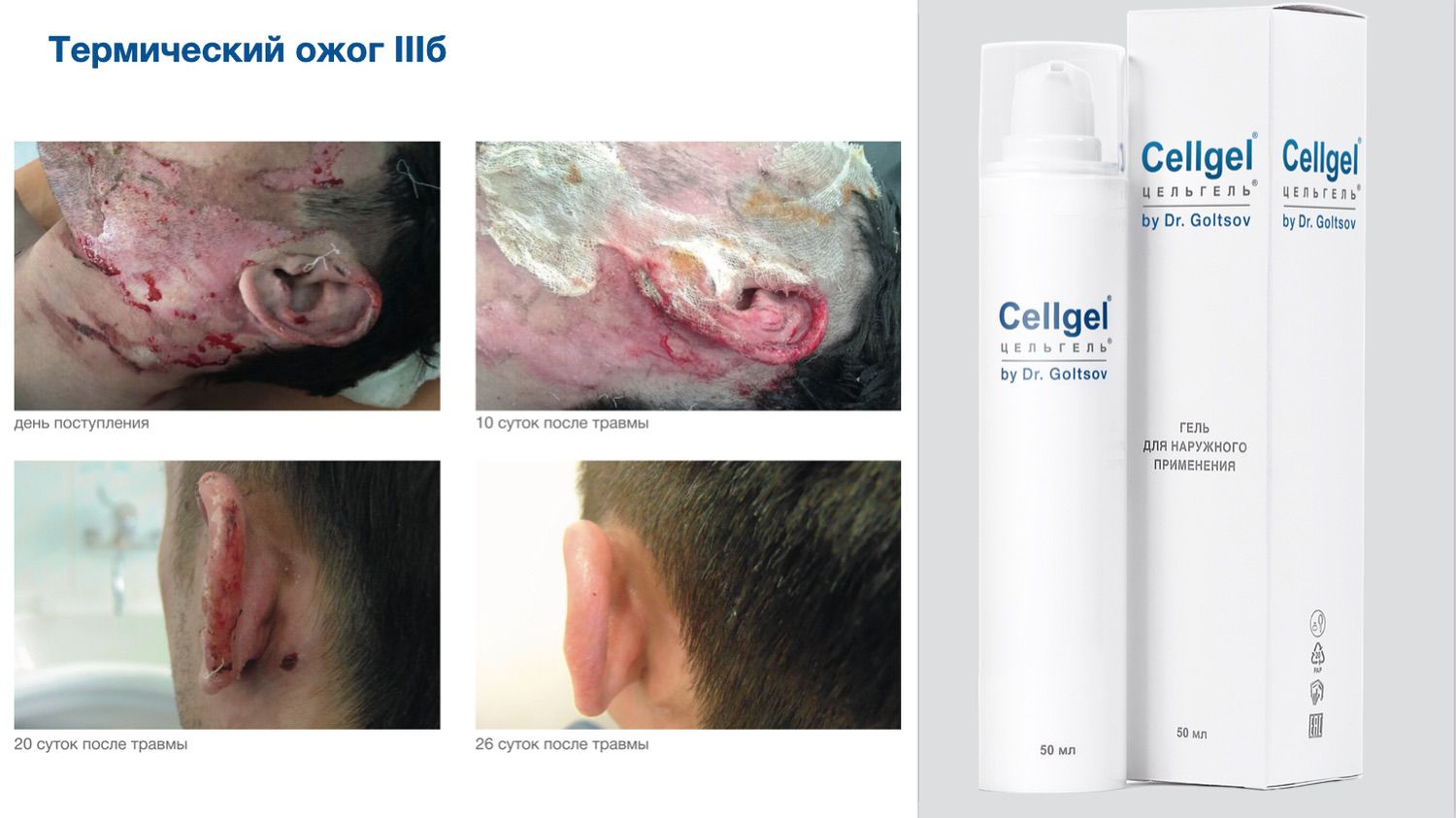
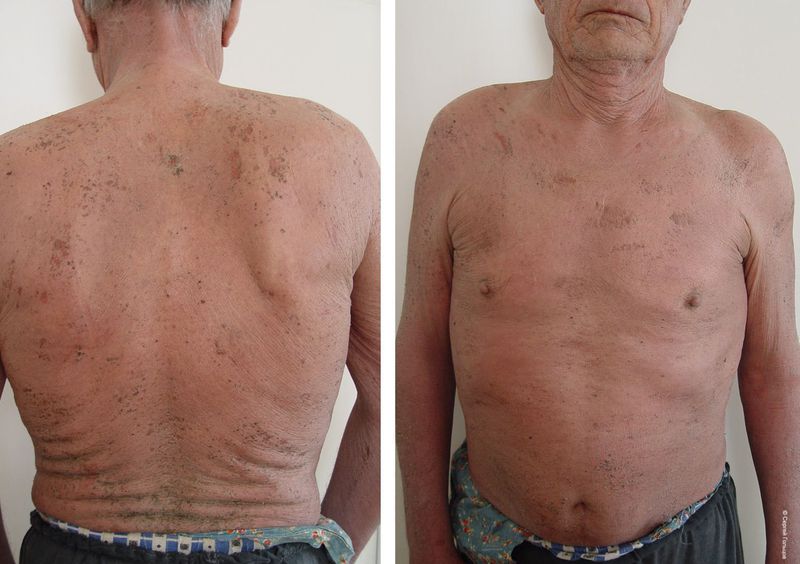
Цельгель искусственно повышает концентрацию сигнальных молекул в ране, чтобы активировать механизмы репарации и ускорить естественные механизмы регенерации кожи, которые у человека с возрастом ослабевают. Покупайте в клинику, покупайте себе...
Nature, on its evolutionary path, not only creates complex living structures, perfecting them from unicellular to multicellular, but also seeks to prolong their existence, endowing them with a number of properties at different levels (cellular, organ, organismal, population).
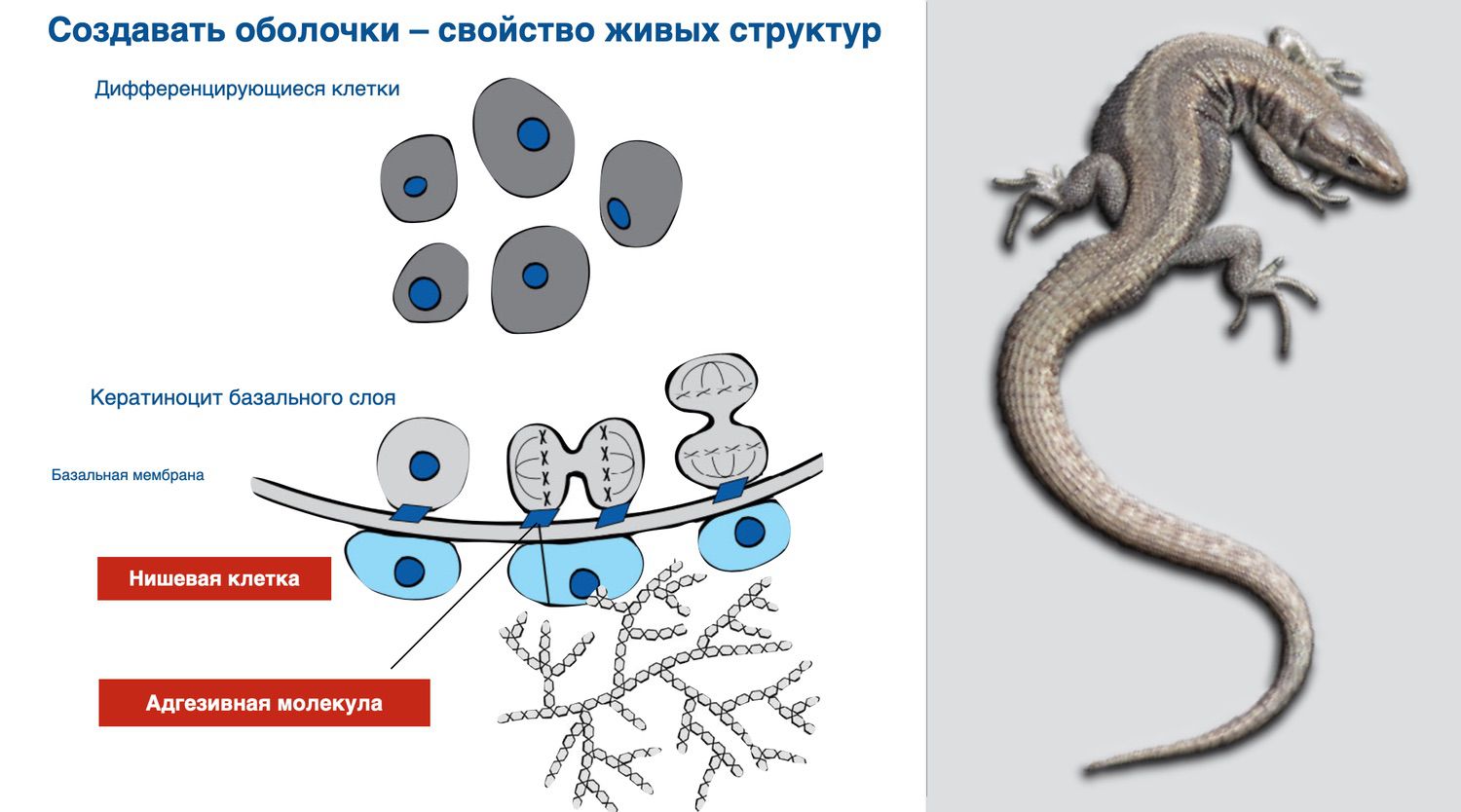
Nature strives for permanence and integrity of living structures, endowing them with the ability to self-reproduce and compensate for damage. Living structures are protected from the external environment by creating envelopes.
Creating membranes is a property of living structures. Human skin is one of them.